During a renal scan, you should measure kidney length, width, the antero-posterior diameter, and volume.
You should also understand cortical thickness and parenchymal thickness.
In routine practice, measuring the length and width of the kidney is usually enough. These measurements should be clearly mentioned in the report.
Volume, cortical thickness, and parenchymal thickness are not measured in every patient. You should measure them only when there is a clinical indication or when kidney disease is suspected.
Renal Length Measurement on Ultrasound
Renal length is the maximum distance from the upper pole to the lower pole of the kidney. It is measured in the longitudinal view. This is the single most important measurement in kidney ultrasound. It best reflects the overall size of the kidney and helps assess chronic kidney disease.
Now let’s understand how to measure it correctly.
Place the probe on the patient’s flank along the mid-axillary line. Keep the probe marker directed toward the head. Slowly adjust the probe until you get the kidney in its maximum length. Both the upper and lower poles must be clearly seen in the same image.
Once you have the correct image, place one caliper at the upper pole of the kidney and the second caliper at the lower pole. Always place the calipers on the renal capsule.
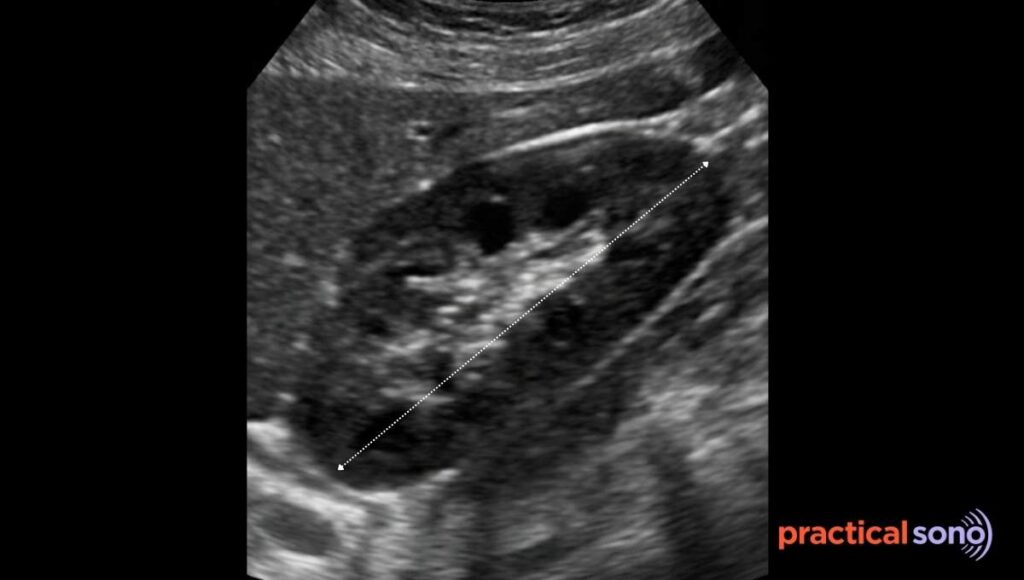
The kidney must be imaged in its true long axis. If you do not adjust the probe properly, you will not get a true longitudinal view. This can make the kidney look falsely small.
If you cannot see the kidney borders clearly, turn on tissue harmonic imaging. Harmonics make the borders sharper. This helps you identify the capsule clearly and place the calipers accurately.
Normal Measurement
Normal adult renal length: 9–12 cm.
Normally, the right kidney is about 2 cm shorter than the left kidney because of the liver.
A difference of more than 2 cm between the two kidneys is considered abnormal.
Normal renal length in pediatric
Newborn (term): 4.0 – 4.5 cm
0–3 months: 4.5 – 5.5 cm
3–12 months: 5.5 – 6.5 cm
1–2 years: 6.0 – 7.0 cm
2–5 years: 6.5 – 8.0 cm
5–10 years: 8.0 – 9.5 cm
10–15 years: 9.0 – 11.0 cm
≥ 15 years: 9 – 12 cm
In children, both kidneys should be similar in size. A side-to-side difference of more than 1 cm is considered abnormal.
The left kidney is usually slightly longer than the right kidney. Premature infants normally have smaller kidneys compared to term infants.
Height-based charts are more accurate than age-based charts, especially after infancy. When evaluating kidney length in children, always correlate the measurement with the child’s age, height, and clinical context.
Enlarged Kidney
A kidney is considered enlarged when its size is more than the expected normal range for that patient and the finding matches the clinical context.
In adults, a kidney is considered enlarged when the renal length is more than 12 cm. Enlargement is also suspected when there is a clear size difference compared to the opposite kidney. A difference of more than 2 cm is abnormal.
Kidney width and thickness also help in assessment. A width significantly more than 4 to 6 cm or a thickness more than 3 to 5 cm suggests enlargement.
Renal volume is another important indicator. A volume greater than 190 mL in men or greater than 150 mL in women strongly suggests renomegaly.
A kidney should never be labeled “enlarged” based on length alone without considering:
- Patient height and body habitus
- Age
- Pregnancy
- Hydration status
- Clinical scenario
The term “enlarged kidney” is more confidently used when increased length is accompanied by:
- Increased renal width and AP diameter
- Bulky appearance of kidney
- Preserved or increased parenchymal thickness
- Normal or mildly increased cortical thickness
Physiological Causes of Enlarged Kidney
Some causes of kidney enlargement are physiological and not related to disease.
Compensatory hypertrophy occurs when one kidney is absent or not functioning properly. In this situation, the healthy kidney grows to handle the extra workload. It can increase up to one and a half times its normal size.
Pregnancy is another physiological cause. During pregnancy, it is common for the kidneys to increase in overall size. There may also be mild dilation of the collecting system due to normal hormonal and mechanical changes.
Pathological Causes of Enlarged Kidney
- Hydronephrosis
- Acute Pyelonephritis
- Acute glomerulonephritis
- Acute tubular necrosis
- Early diabetic nephropathy
- Polycystic Kidney disease
- Acute renal vein thrombosis
- Malignancy
Small Kidney
A kidney length of less than 8 cm suggests a small and shrunken kidney. This usually indicates chronic kidney disease with fibrosis.
Cause of Renal Atrophy/Shrunken Kidney:
- Congenital: Renal Hypoplasia, Renal Dysplasia
- Chronic Kidney disease
- Renal artery stenosis
- Chronic Pyelonephritis
- Reflux nephropathy
Renal Width Measurement on Ultrasound
Renal width is the maximum transverse diameter of the kidney. It is measured in the transverse view at the level of the renal hilum.
To measure it correctly, scan the kidney in a transverse section at the level of the renal hilum.
First, get longitudinal view of kidney in mid axillary line and then rotate the probe anticlockwise. The probe marker should face downward toward the spine.
Identify the widest part of the kidney, usually at hilum.
Place the calipers from the outer edge of the medial cortex to the outer edge of the lateral cortex. Make sure the probe is perpendicular to the long axis of the kidney. This prevents underestimation of the width.
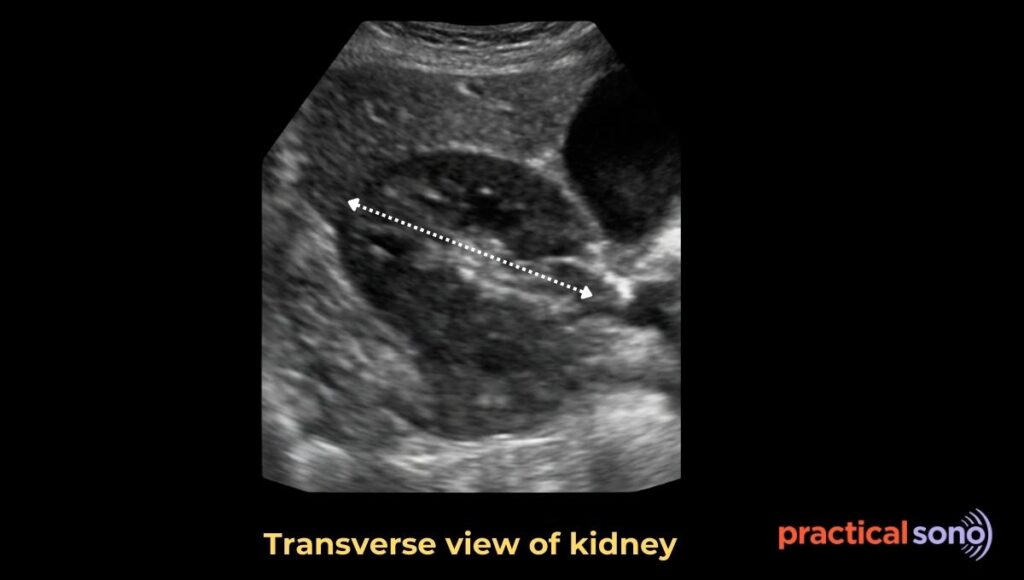
In adults, the average renal width is about 4 to 6 cm. You do not need to memorize this number. A simple rule is that the kidney width is usually about half of its length.
Renal AP thickness (anteroposterior diameter)
Renal Antero-Posterior Thickness is the maximum anteroposterior dimension of the kidney. It is measured in the transverse plane.
To measure it correctly, obtain a true transverse section of the kidney, usually at the level of the renal hilum. The probe marker should face downward. Measure from the anterior outer renal capsule to the posterior outer renal capsule.
Take the measurement perpendicular to the renal width. Avoid oblique sections because they can falsely increase or decrease the AP diameter.
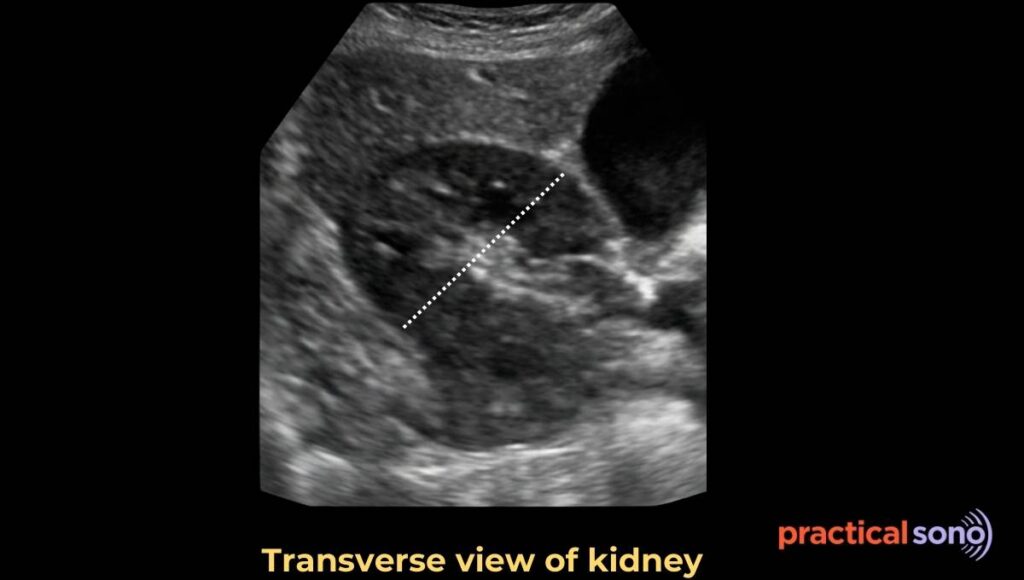
In adults, the average renal AP diameter is about 3 to 5 cm. AP thickness alone has limited value. It is mainly used to help estimate the overall renal size and calculate renal volume.
Renal Volume
Renal volume represents the overall size of the kidney. It correlates better with renal mass than any single linear measurement. However, in routine adult renal ultrasound, renal volume is not measured regularly.
Renal volume reflects functional renal parenchymal mass more accurately than renal length alone.
Now let’s understand when renal volume should be measured.
Renal volume should be measured when a precise assessment of kidney size is clinically important.
This includes renal transplant evaluation and follow-up. It is also useful in pediatric patients because volume correlates better with age and body surface area.
In chronic kidney disease, renal volume helps when detailed documentation of renal mass is needed. It is also measured in research studies or during serial follow-up when small size changes matter.
Renal volume is important in congenital anomalies, dysplastic kidneys, and unilateral kidney disease to compare functional renal mass.
Now let’s see how renal volume is calculated.
Renal volume is calculated using the ellipsoid formula.
Renal volume = Length X width X AP diameter X 0.523.
You do not need to memorize this formula. It is already built into your ultrasound machine. To calculate renal volume, press the measure button and select kidney volume. Then start taking the required measurements.
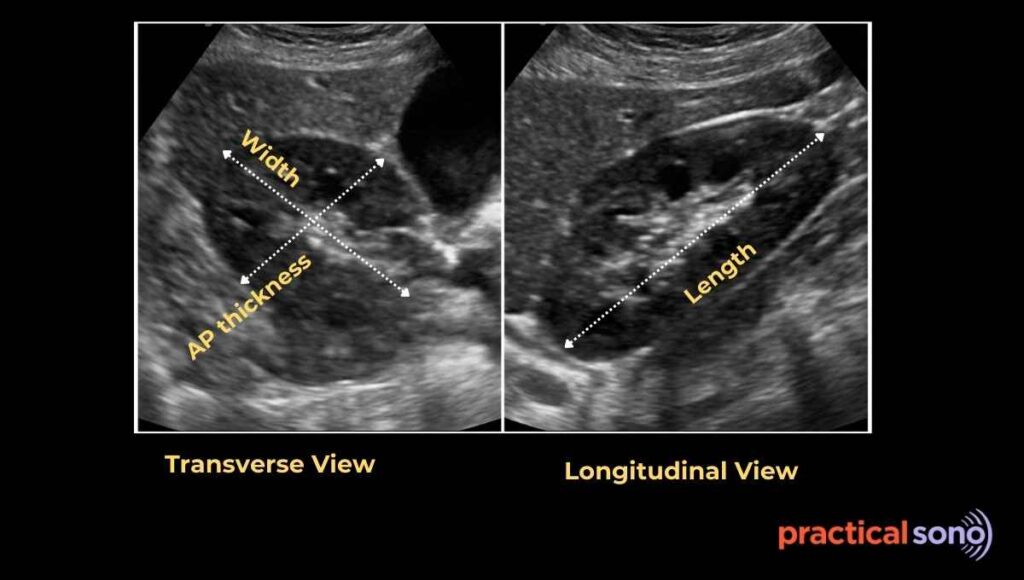
First, measure the renal length in the true longitudinal plane from upper pole to lower pole. Next, measure the renal width in the transverse plane at the level of the renal hilum. Then measure the renal AP diameter in the same transverse plane.
Once all three measurements are completed, the machine will automatically calculate the renal volume.
Always calculate the volume of each kidney separately.
Normal adult renal volume is approximately:
Male: 120–200 ml per kidney
Female: 90–170 ml per kidney
Total combined renal volume is usually around 250–400 ml.
Reduced renal volume suggests chronic irreversible renal disease and loss of nephron mass.
Enlarged renal volume may be seen in acute inflammatory conditions, obstruction, pregnancy, or early diabetic nephropathy.
Marked asymmetry in renal volume indicates chronic unilateral disease.
Renal Cortical Thickness on Ultrasound
Renal cortical thickness is the distance from the outer renal capsule to the base of a medullary pyramid. It represents true cortical tissue, which contains most of the functioning nephrons.
Let’s understand how to measure it correctly.
Cortical thickness is measured in the longitudinal plane of the kidney. Obtain a clear longitudinal image showing a well-defined medullary pyramid. Place one caliper on the outer renal capsule. Place the second caliper at the base of the medullary pyramid, not at the tip. Measure perpendicular to the capsule.
Always take the measurement at the mid-pole of the kidney, where the cortex is best seen. Avoid measuring over the renal columns or at the poles, as this can give inaccurate values.
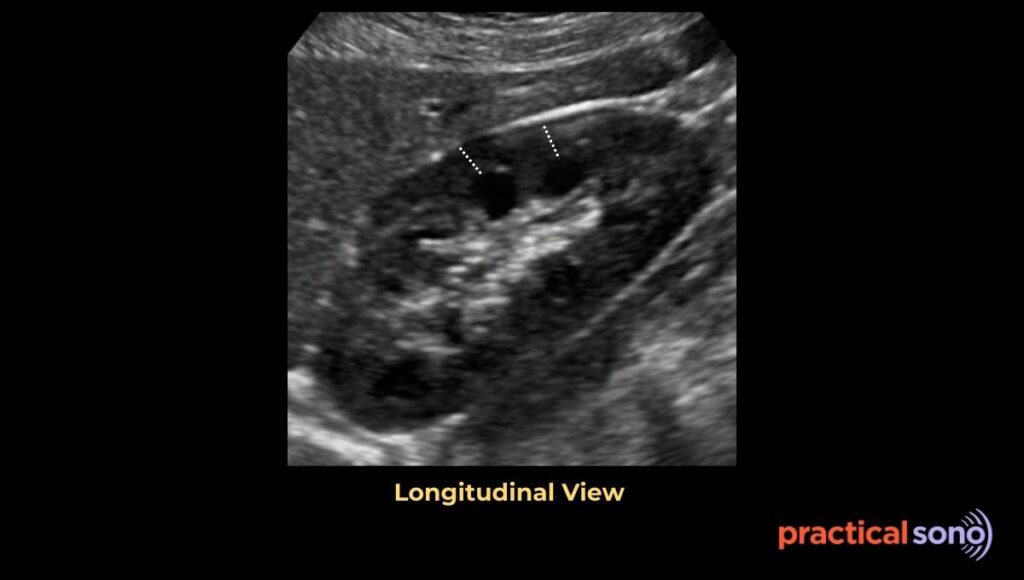
In adults, the normal renal cortical thickness is about 6 to 10 mm. It may be slightly lower in elderly patients. A cortical thickness of less than 6 mm suggests advanced chronic kidney disease.
Now let’s discuss when cortical thickness should be measured.
It should be measured when chronic kidney disease is suspected. It is also important in medical renal disease, long-standing obstruction, reflux nephropathy, hypertensive nephropathy, and diabetic nephropathy.
Cortical thickness is useful during follow-up of patients with known chronic kidney disease.
Reduced cortical thickness indicates chronic and irreversible renal damage and correlates with reduced renal function. Cortical thinning is often a better marker of chronicity than renal length alone.
If cortical thickness is preserved but echogenicity is increased, this may suggest earlier stages of medical renal disease.
Cortical thickness should be reported when chronic kidney disease or medical renal disease is suspected. In normal kidneys with normal length and normal echogenicity, it is not necessary to mention cortical thickness.
Renal Parenchymal Thickness on Ultrasound
Renal parenchymal thickness is the distance from the renal capsule to the renal sinus fat.
It represents the combined thickness of the renal cortex and medulla. Measuring it helps assess the chronicity and severity of kidney disease, especially in obstructive conditions.
To measure it correctly, obtain a longitudinal image of the kidney through the mid-pole. Identify the bright echogenic renal sinus in the center.
Place one caliper on the outer renal capsule and the second caliper on the outer margin of the renal sinus fat. Measure perpendicular to the capsule. Avoid measuring at the poles or over the columns of Bertin.
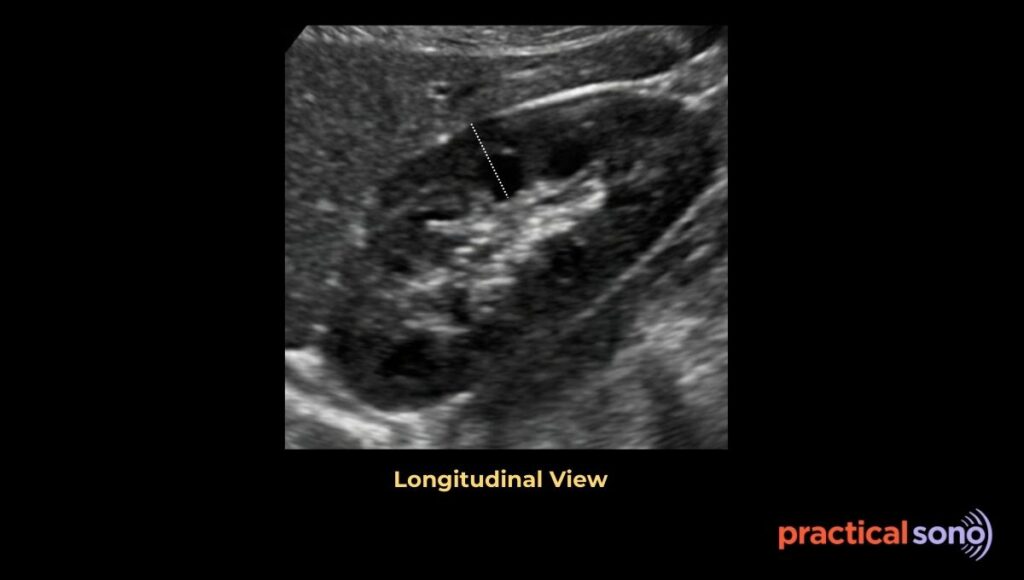
In adults, normal renal parenchymal thickness is about 15 to 20 mm.
Renal parenchymal thickness should be measured in cases of suspected chronic kidney disease, chronic or long-standing hydronephrosis, reflux nephropathy, follow-up of obstructive uropathy, evaluation of renal transplant function, or when renal length is borderline.
Reduced parenchymal thickness suggests chronic kidney damage and correlates with decreased renal function.
In obstructive uropathy, progressive thinning indicates chronic disease and poor recovery. Preserved parenchymal thickness with pelvicalyceal dilatation usually favors acute obstruction.