Finding appendicitis on ultrasound is not easy. In about 20 to 30 percent of cases, you will not see an enlarged appendix. This can happen for many reasons. The abdomen may be full of gas. The appendix may be in an unusual position. And that is totally okay.
But when you know where to look for the appendix during scanning, it becomes much easier. When you understand how each stage of appendicitis looks on ultrasound, your confidence will grow. You will start recognizing the patterns.
In this Appendicitis Ultrasound Protocol guide, you will know how a normal appendix looks on ultrasound. We have explained the pathophysiology in simple words with ultrasound images showing different stages of appendicitis. Also, you’ll get reporting sample to describe your findings with confidence.
Now, let’s start with the anatomy of the normal appendix.
Anatomy of Normal Appendix
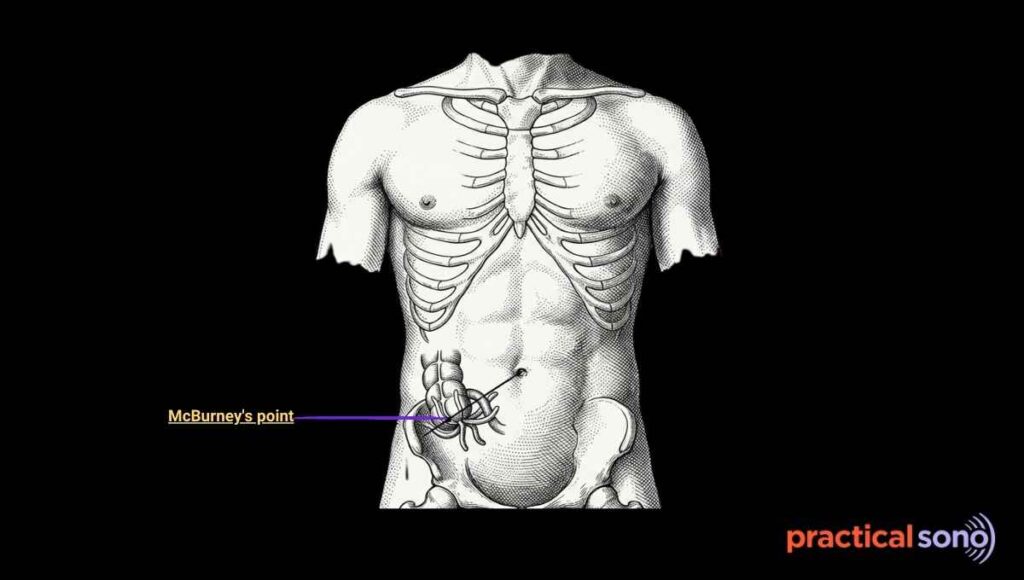
The appendix is a small, narrow, blind-ended, worm-like. It is usually located in the right lower quadrant at McBurney point.
Unlike the small intestine, the appendix does not show peristalsis.
The base of the appendix stays in a fixed location, but the tip can lie in many different positions. The most common position is retrocecal, where the appendix lies behind the cecum.
It may also be pelvic, where it extends down into the pelvis. In the subcecal position, it lies below the cecum. It can also be pre-ileal or post-ileal, lying in front of or behind the terminal ileum.
The appendix arises from the posteromedial wall of the cecum. This is usually about 2 cm below the ileocecal valve.
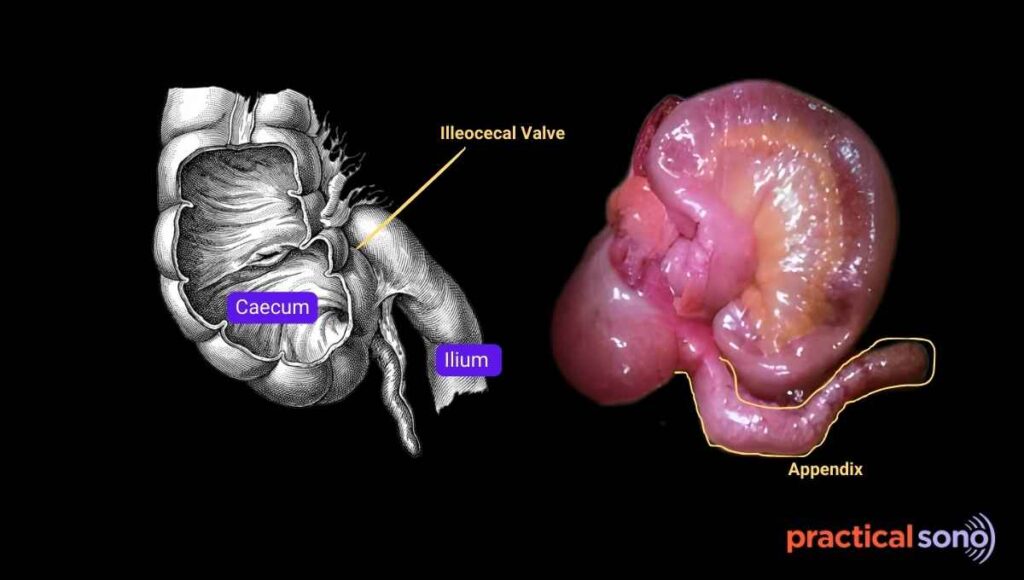
Normal Measurement:
- Length: 8 to 10cm
- Outer to Outer wall diameter: Less than 6mm
- Wall thickness: Less than 3mm
A small triangular fold of peritoneum called the mesoappendix connects the appendix to the mesentery of the terminal ileum.
It carries the blood vessels and nerves that supply the appendix.
Ultrasound Appearance of Normal Appendix
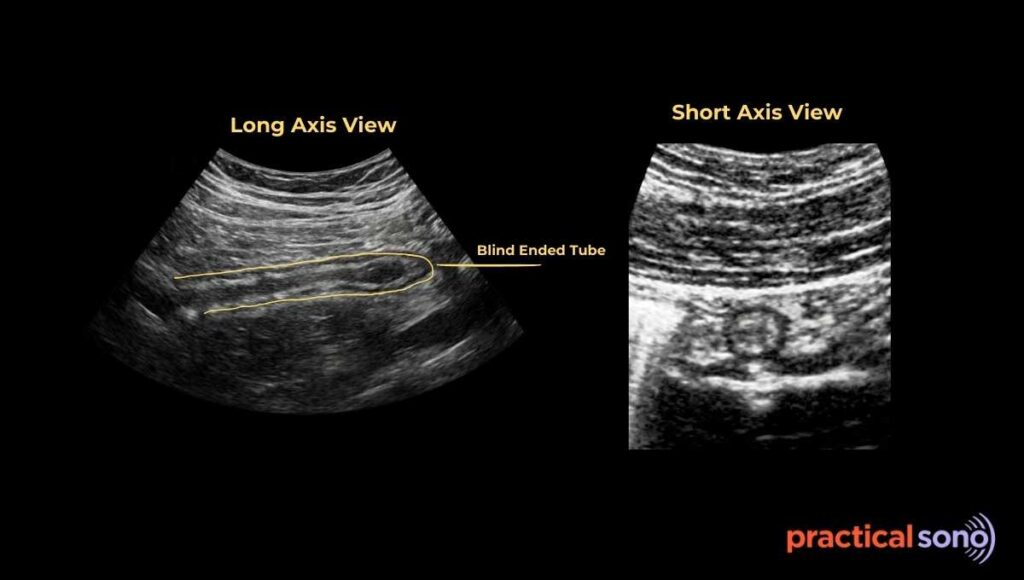
On ultrasound, the appendix appears as a blind-ended, tubular, non-peristaltic structure on the longitudinal view.
A normal appendix is compressible.
To confirm that you are seeing the appendix, always look for the blind end.
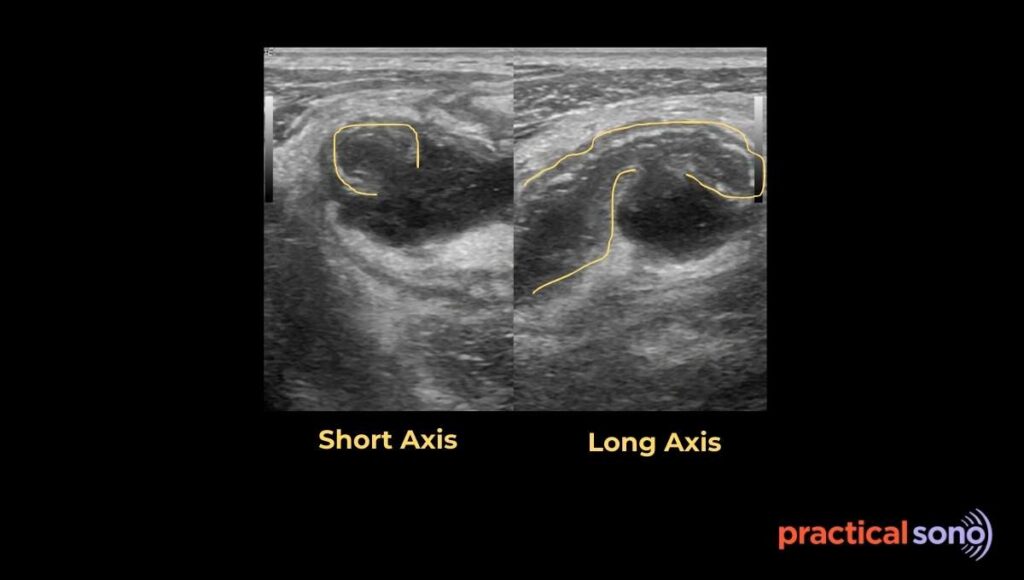
On the transverse or short-axis view, the appendix appears as a perfectly circular or ovoid structure. When you apply pressure with the probe, it should easily compress or disappear.
Important Landmark for finding Appendix: Psoas Muscle and Iliac Vessels
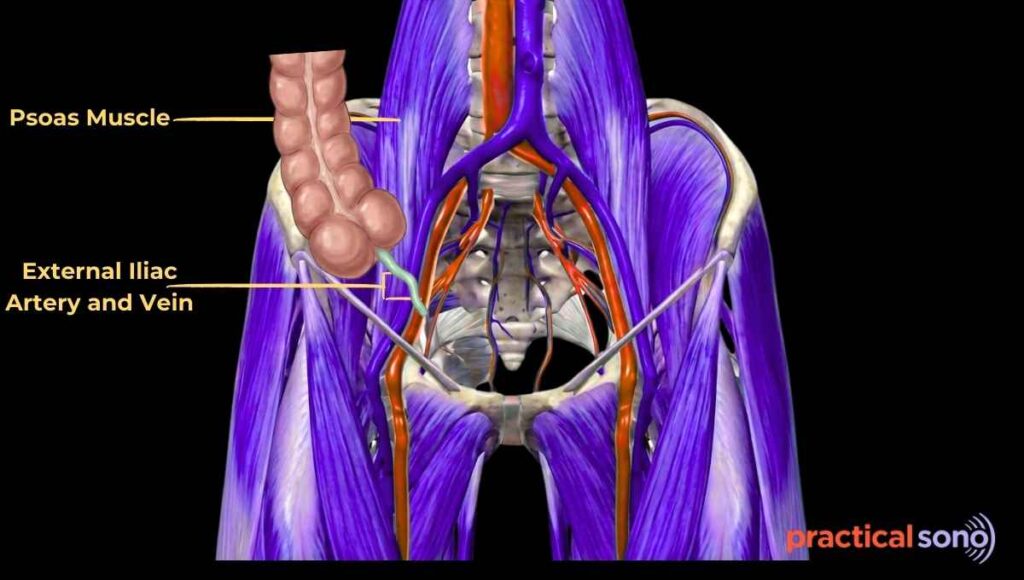
The relationship between the appendix, the psoas muscle, and the iliac vessels is considered the gold standard landmark for finding the appendix on ultrasound.
The psoas muscle and the external iliac vessels form the posterior boundary, or the floor, of the right iliac fossa.
Appendix usually lies anterior to these structures. This means it sits on top of the psoas muscle and the iliac vessels.
The psoas muscle appears as a large, hypoechoic, almond-shaped structure. You will see internal bright streaks that represent muscle fibers.
The iliac vessels appear as anechoic, black, tubular structures. The artery shows pulsation, while the vein is compressible.
On the longitudinal view, a normal or mildly inflamed appendix often looks like a snake or a tube crawling over the external iliac vessels.
To see the appendix clearly, graded compression is very important.
You gently press the ultrasound probe downward toward the psoas muscle.
The goal is to pin the appendix against this firm muscle. If the appendix is normal, it will flatten when you apply pressure.
If the appendix is inflamed, as in appendicitis, it will stay round and non-compressible. It will appear like a target sitting directly on top of the psoas muscle.
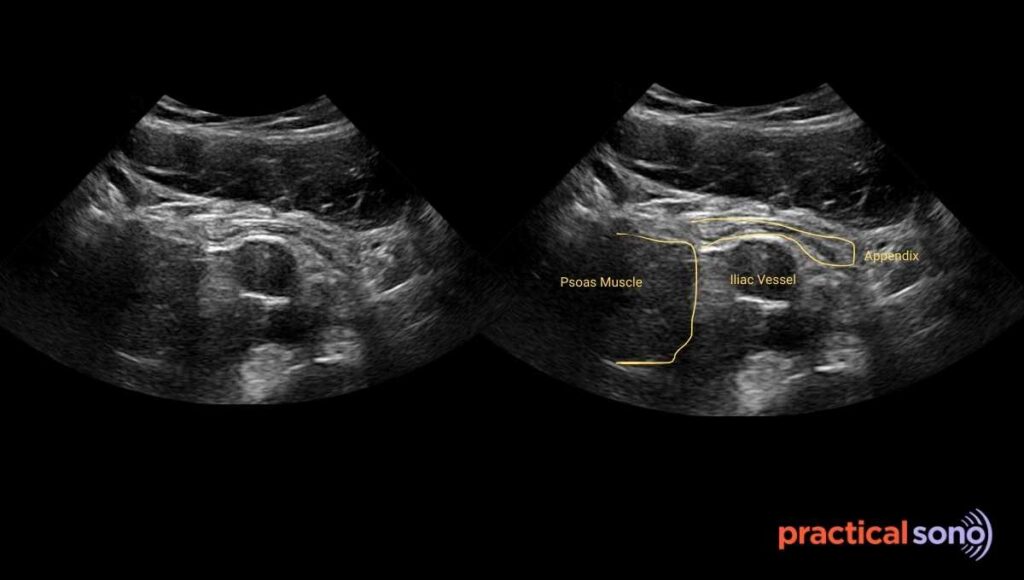
“The “Sandwich” View: Look for Appendix in between Anterior Abdominal Wall Muscle and Psoas Muscle
When you scan the right lower quadrant in the transverse plane, think of the appendix as being sandwiched between two layers.
The top layer, or the ceiling, is the abdominal wall. This is the first structure the ultrasound beam meets.
You will see the skin and subcutaneous fat as a bright outer layer, followed by the abdominal muscles. You must scan through these layers to reach the appendix.
The middle layer is the right iliac fossa. This is where the appendix seen. Your job is to find the blind ended-tubular structure in this area.
The appendix is not very deep. You should look for a tubular structure close to the anterior abdominal wall.
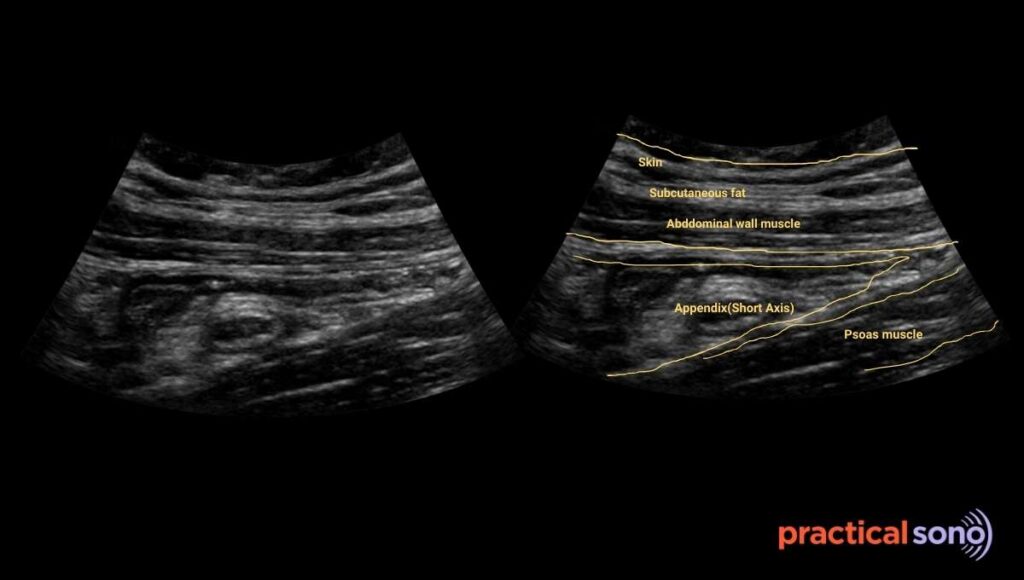
This area often contains distractors.
The cecum is usually just above or to the side of the appendix. It often contains gas, which causes dirty shadowing. You must use graded compression to push this gas away.
The terminal ileum is also nearby.
Unlike the appendix, it shows peristalsis and is open at both ends. The appendix appears as a round target sign in this space.
The bottom layer, or the floor, is formed by the psoas muscle and the external iliac vessels.
This is the most important part of the sandwich.
It gives you a firm surface to scan against.
The psoas muscle appears as a large, almond-shaped, hypoechoic structure and acts like a backboard. The external iliac artery and vein lie just medial to or on top of the psoas. The artery pulsates, and the vein is compressible.
These posterior structures are fixed against the pelvic bone.
This firmness allows you to pin the appendix in place. Without this solid floor, the appendix would simply move deeper when you press, making diagnosis and measurement very difficult.
To find appendix, first find the psoas muscle and the iliac vessels.
Once you see them, you know you are scanning deep enough. Then slowly apply pressure with the probe.
Your goal is to make the ceiling meet the floor.
Now watch what happens in the middle layer.
In a normal case, as you press, bowel gas in the cecum moves away.
The normal appendix flattens and gets squashed against the psoas muscle.
In appendicitis, the cecum may move, but the appendix stays round. It remains stuck on top of the psoas or iliac vessels. It cannot be compressed because it has become a high-pressure, fluid-filled tube.
Gut Signature of the Appendix and How It Differs From the Small Intestine
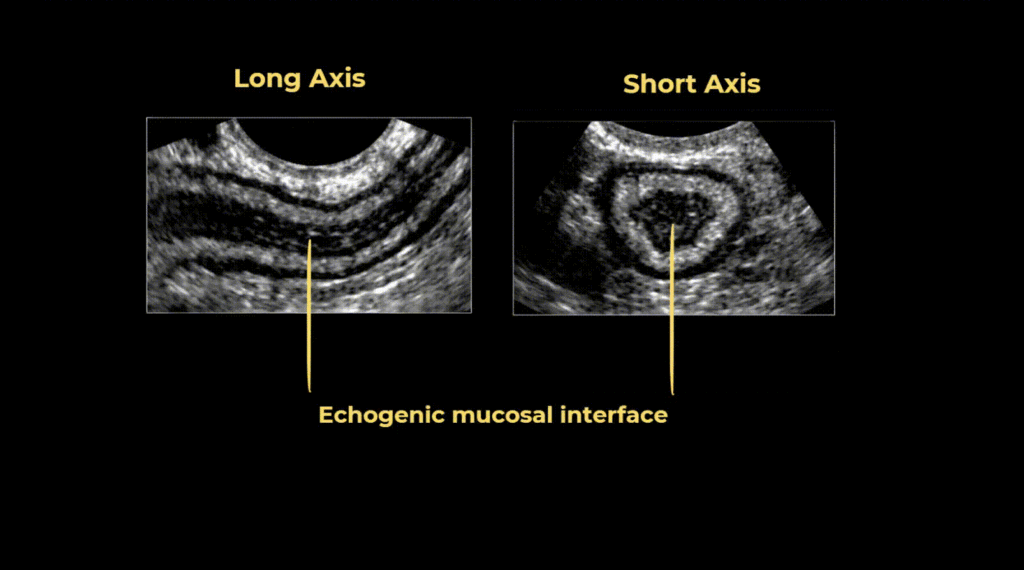
The gut signature refers to the layered appearance of the bowel wall on ultrasound.
The appendix has a classic gut signature made of five layers.
You must know these layers and learn to identify them on ultrasound. This is very important, especially for detecting gangrenous appendicitis.
The first layer is the interface or superficial mucosa. It appears echogenic or bright. This layer represents the boundary between the lumen and the wall.
The second layer is the mucosa or deep mucosa. It appears hypoechoic or dark. This layer contains lymphoid follicles, which are prominent in the appendix.
The third layer is the submucosa. It is echogenic and very bright. This is the key layer and is usually the most visible ring. Loss of this bright layer is a strong sign of perforation.
The fourth layer is the muscularis propria. It appears hypoechoic and dark. This is the main muscle layer, and it becomes significantly thickened in appendicitis.
The fifth layer is the serosa or subserosal fat. It appears echogenic and forms the thin outer skin of the appendix.
The lumen of the appendix is much narrower than that of the small intestine. It often looks irregular or star-shaped.
This is different from the small bowel, which has a smooth and wider lumen. Because the appendix lumen is narrow, it is more prone to obstruction.
As the appendix becomes obstructed and inflamed, the wall layers become more obvious.
You will see alternating bright and dark rings. The submucosa usually stays bright and may become slightly thickened. The muscularis layer becomes thick and dark due to swelling. This creates the classic bull’s-eye or target sign on the transverse view.
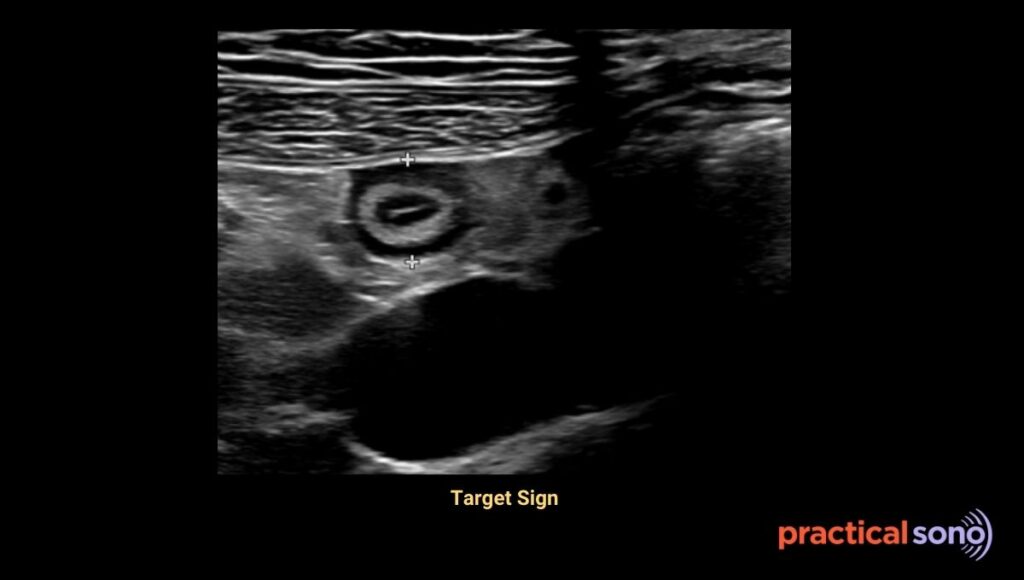
When the disease progresses to ischemia and gangrene, the normal layered appearance is lost.
This happens because tissue death causes the normal boundaries between layers to break down. This finding is a red flag and suggests an impending perforation.
This is called loss of stratification. The layers become blurred, fuzzy, or may disappear completely.
In perforation, you may see a clear defect in the bright submucosal layer. Once this echogenic ring is broken, infected contents leak out into the surrounding space.
This confirms rupture and represents a surgical emergency.
Pathophysiology of Appendicitis And Ultrasound Images of Different Stages
Step 1: Luminal Obstruction (The Trigger)
A physical blockage occurs at the opening of the appendix. This is the starting point of appendicitis. Common causes include an appendicolith, which is a hard fecal stone.
It can also be caused by lymphoid hyperplasia, which is common in children, or by parasites.
On ultrasound, an appendicolith appears as a bright hyperechoic structure inside the lumen. It produces a sharp posterior acoustic shadow.
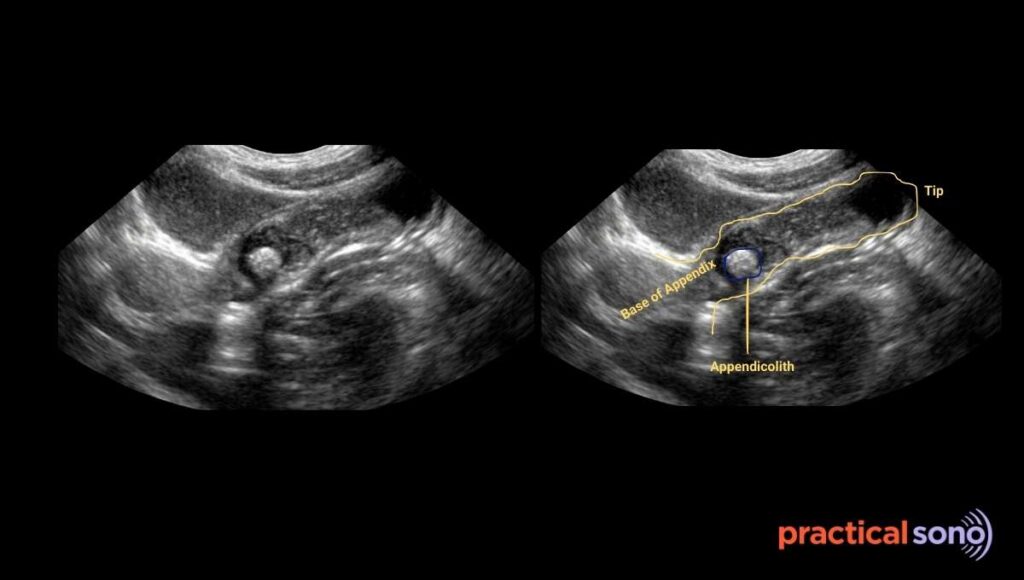
Step 2: Distension and Bacterial Overgrowth
Mucus production continues behind the blockage but cannot escape. Pressure builds up inside the appendix. This causes the appendix to stretch and enlarge. Bacteria start multiplying in the trapped fluid.
On ultrasound, the diameter becomes more than 6 mm. The appendix looks like a blind ending tube. Because it is under pressure, it does not compress when you press with the probe.
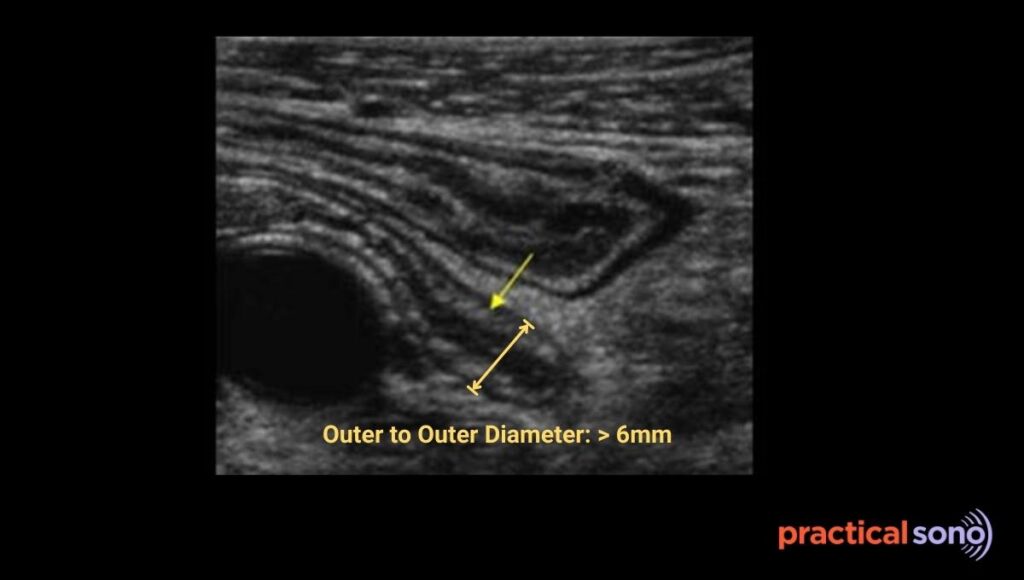
Step 3: Venous and Lymphatic Congestion Edema
As pressure keeps rising, it becomes higher than the pressure in the small veins and lymphatic vessels of the appendiceal wall. These vessels collapse. Fluid then leaks into the wall layers, causing edema.
On ultrasound, the wall thickness becomes more than 3 mm. In the transverse view, the appendix shows a target sign. It looks like a bull’s eye. You see a dark hypoechoic wall layer caused by fluid in the muscle.
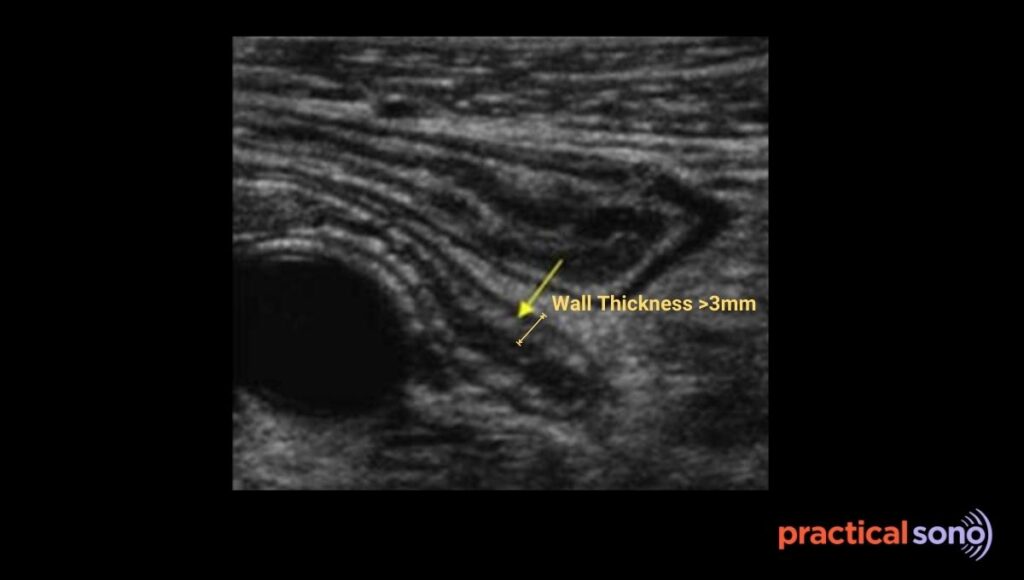
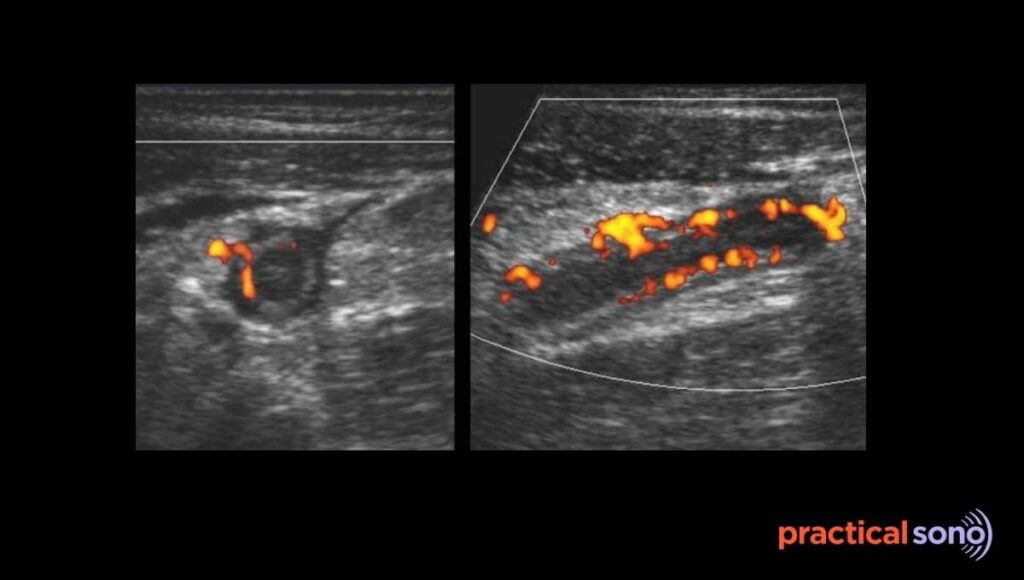
Step 4: Arterial Hyperemia Active Inflammation
The body reacts to infection by widening nearby arteries. This helps bring more white blood cells to fight the infection. This process is called hyperemia.
On ultrasound, color Doppler shows increased blood flow in the appendiceal wall. The wall looks very vascular. If the diameter is less than 6 mm but you see increased Doppler flow, this may indicate very early appendicitis.
Step 5: Suppuration and Periappendiceal Fat Stranding
At this stage, inflammation spreads through the appendiceal wall into the surrounding peri vesical fat. The disease has now progressed beyond simple obstruction and edema. Pus begins to form inside and around the appendix. This process is called suppuration.
The mesoappendix, which is the fat and connective tissue that supports the appendix, reacts to this irritation. Blood vessels inside this fat dilate. Fluid called exudate leaks into the fat cells, causing swelling and inflammation.
The omentum, often called the policeman of the abdomen, may move toward the inflamed appendix. It tries to wrap around the appendix to contain the infection. This adds more fat to the inflamed area and helps limit the spread of disease.
On ultrasound, normal mesenteric fat usually looks dark or mildly gray with a fine, lacy appearance. When the fat becomes inflamed, it turns bright white or hyperechoic. The fat loses its sharp borders and appears hazy, smudged, or dirty. This happens because fluid collects between fat lobules, creating many surfaces that reflect the ultrasound beam.
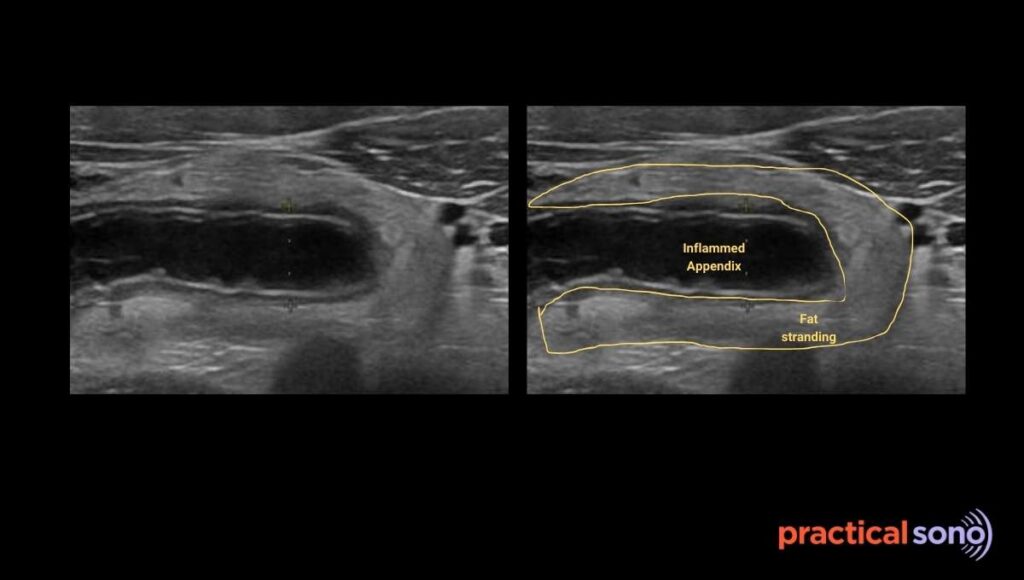
This appearance is called periappendiceal fat stranding. The normally dark fat becomes bright and unclear. You may also see nearby reactive lymph nodes that appear enlarged.
Step 6: Ischemia and Gangrene Tissue Death
This is a critical and irreversible stage of appendicitis. At this point, the pressure inside the appendix becomes higher than the arterial blood supply. Blood can no longer reach the wall. The tissue begins to die. This stage is a true surgical emergency, and rupture can occur within hours.
In earlier stages, only the low pressure veins collapse. In this stage, the pressure from trapped pus finally exceeds the high pressure arterial flow. This leads to ischemia, meaning the wall becomes deprived of oxygen. Without oxygen and nutrients, the smooth muscle and connective tissue die. This process is called necrosis and results in gangrene.
Dead tissue allows bacteria to spread quickly. Gas forming bacteria invade the appendiceal wall and worsen the damage.
On ultrasound, the most reliable sign of gangrene is loss of mural stratification. Normally, you can see five distinct gut wall layers. In gangrene, these layers disappear. The wall looks fuzzy, uniformly dark, or poorly defined. This happens because the normal structure of the wall is destroyed by necrosis.
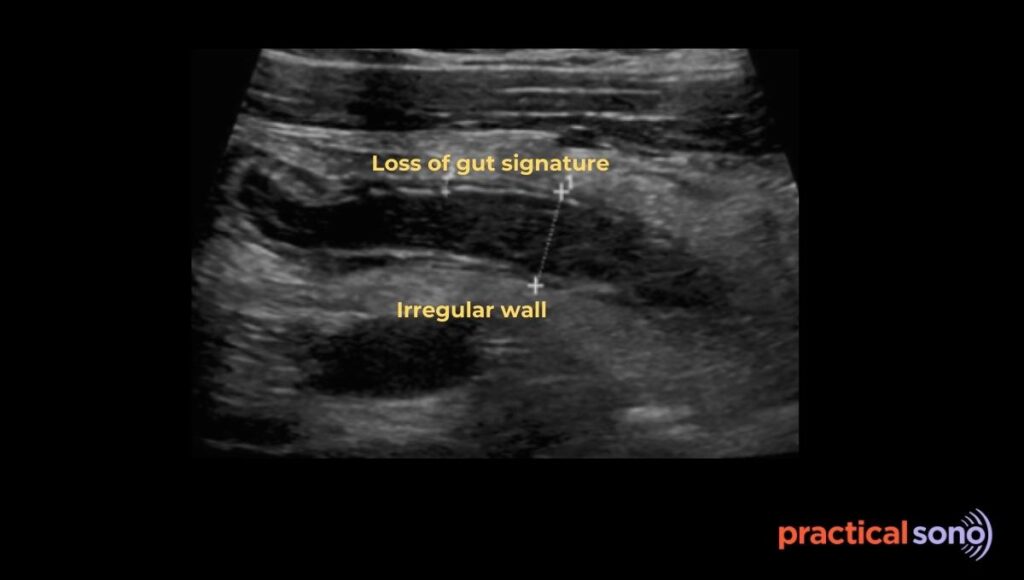
The bright submucosal layer, often called the safety line, is no longer visible. When this line is gone, rupture is very close.
Color or power Doppler provides definitive confirmation. There is no blood flow in the appendiceal wall. The wall is avascular because the arterial supply is completely cut off. This finding is very different from the earlier hyperemic stage, where blood flow was increased. A non compressible appendix larger than 6 mm with no Doppler flow is a major warning sign of advanced disease.
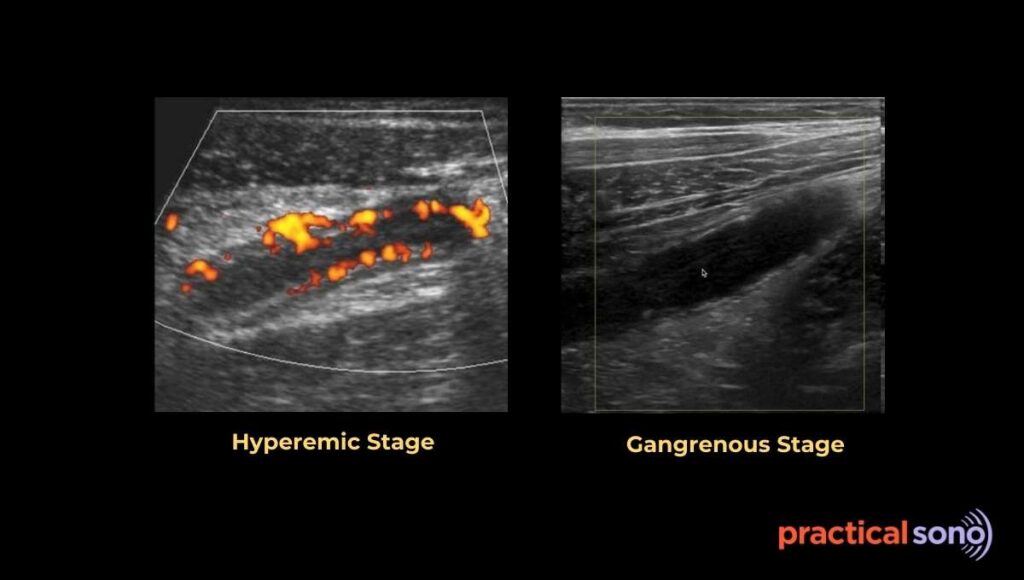
You may also see associated findings. Pneumatosis may be present due to gas produced by bacteria inside the dead wall. On ultrasound, this appears as tiny bright white spots or dirty shadowing within the wall. Free fluid is usually seen around the appendix or in the pouch of Douglas. This happens because the dying tissue leaks fluid into the surrounding area.
Step 7: Perforation Rupture
This is the final and most dangerous stage of appendicitis. The necrotic wall can no longer tolerate the rising pressure and finally breaks open. This usually occurs within 24 to 48 hours after symptoms begin. At this moment, a localized infection turns into a potentially life threatening condition.
Perforation is the direct result of gangrene. The appendix has lost its strength and structure. Internal pressure overwhelms the dead tissue, leading to rupture.
Structural Collapse of the Appendix
As pressure continues to build, the appendix behaves like a pressure cooker. The weakest part of the wall, often the mid portion or the tip where blood supply is poorest, tears open. Infected material such as pus, bacteria, and sometimes the appendicolith spill into the peritoneal cavity.
There may be a short period of pain relief after rupture. This happens because the pressure inside the appendix suddenly drops. This is a dangerous sign. Severe pain usually returns soon after as generalized peritonitis develops.
Ultrasound Finding The Deflated Appendix
After perforation, the appendix often becomes difficult to identify. Once it ruptures, it decompresses. The previously round and tense appendix may now look collapsed, irregular, or deflated. It is no longer perfectly circular because the internal pressure is gone.
Because it is no longer distended, the appendix may be hard to see. If you previously identified a 10 mm appendix and later only see a poorly defined 6 mm structure, you should strongly suspect perforation.
Ultrasound Finding The Break in the Line
This is the most specific sign of rupture when it is visible. Focus on the bright submucosal layer, also called layer three. You may see a clear gap or break in this bright white line. This represents a full thickness defect in the wall where contents have leaked out.
Secondary Ultrasound Signs of Perforation
After rupture, indirect findings become very important because the appendix itself may be hidden. You may see loculated free fluid near the appendix or in the pouch of Douglas. This fluid may be simple or complex and represents spilled pus.
Extraluminal gas may be seen as bright white spots in the surrounding fat. These produce dirty acoustic shadowing. If an appendicolith is seen outside the appendix within the fat, this is definitive proof of perforation.
Another key sign is the avascular tip. If the tip of the appendix looks ill defined and shows no Doppler flow, this is the most likely site of rupture.
Step 8: Abscess or Phlegmon Formation
This is the final stage of complicated appendicitis. It represents the body’s last defense mechanism after perforation. The goal is to contain a life threatening infection and prevent it from spreading through the entire abdomen.
Once the appendix ruptures, infected material such as feces, bacteria, and pus spills into the normally sterile peritoneal cavity. The body immediately tries to isolate this contaminated area and quarantine it.
The Phlegmon Phase
A phlegmon is the early response. It is an unorganized and solid inflammatory mass. The omentum and nearby loops of small bowel move toward the rupture site. They stick to the area and to each other, forming a protective barrier. This creates a dense inflammatory clump but without a fluid center.
On ultrasound, a phlegmon appears as an ill defined hypoechoic and heterogeneous area in the right iliac fossa. There is no clear liquid collection yet. Instead, you see bright, hazy inflamed fat and thickened bowel loops that do not move. The sliding sign is lost because the structures are stuck together.
Note: Instead of Phlegmon, use term inflammatory mass.
The Abscess Phase
If the body successfully traps the infection, the center of the phlegmon begins to liquefy. A fibrous wall forms around it. This creates a localized, pressurized pocket of pus called an abscess. While this limits widespread peritonitis, it leaves behind a dangerous localized source of infection.
On ultrasound, an abscess appears as a complex fluid collection. Unlike a simple cyst, it is not black. You see low level gray echoes from pus, debris, and sometimes thin internal septations.
Gas forming bacteria may be present. This creates bright white air foci within the fluid. These produce dirty acoustic shadowing and may form an air fluid level.
Color Doppler is very helpful. The center of the abscess shows no blood flow because it is filled with pus. The wall of the abscess shows increased blood flow. This reflects the body’s attempt to bring immune cells to the edge of the infection.
Where to Look for Abscesses
Always scan common collection sites. The right iliac fossa is the most frequent location, close to the ruptured appendix. The pouch of Douglas is another key area, especially in pelvic appendicitis where gravity pulls pus downward. If the right iliac fossa looks clear but the patient appears very ill, always check this space. In rare subhepatic cases, fluid or abscess may collect in Morison’s pouch near the liver and kidney.
Summary of Ultrasound Findings in Appendicitis
On ultrasound, the appendix appears as a blind ending tubular structure in the right iliac fossa. It is usually seen anterior to the iliac vessels and the psoas muscle.
A key feature is that it is noncompressible when pressure is applied with the probe.
The outer to outer wall diameter is very important. A diameter greater than 6 mm is considered diagnostic for appendicitis. A diameter greater than 8 mm is more definitive. This measurement is highly sensitive but not highly specific.
However, size alone is not always reliable. The normal appendix may be distended with air or fluid. In children, the appendix can be enlarged due to lymphoid hyperplasia. If the diameter is less than 6 mm, appendicitis is very unlikely. However, infection can still be present if secondary signs are seen.
Wall thickness is another key finding. A wall thickness greater than 3 mm is abnormal. The wall layers often appear hypoechoic. In transverse view, the thickened wall forms concentric rings. This creates the classic target sign or bull’s eye appearance.
An appendicolith may be seen. It appears as a bright hyperechoic structure inside the lumen with a posterior acoustic shadow. There is no luminal peristalsis in appendicitis.
Color Doppler shows increased blood flow in the appendiceal wall during active inflammation. In advanced disease, such as necrosis or gangrene, mural stratification is lost and the wall becomes avascular with no Doppler flow.
The periappendiceal region should always be carefully assessed. Inflamed surrounding fat appears bright, hyperechoic, and ill defined. Free fluid or loculated fluid collections suggest perforation or abscess formation.
Always look in the cul de sac or Morrison’s pouch for post appendiceal abscesses. Phlegmon or abscess may be seen in complicated cases. A thickened cecal wall or reactive lymph nodes may also be present. Several complications can occur.
In gangrenous appendicitis, the wall detail is poor, there is no hyperemia, and pneumatosis may be seen within the wall.
A perforated appendix is often difficult to visualize. It usually occurs within 24 to 48 hours after symptom onset and is seen in about 20 to 40 percent of cases. Diagnosis is challenging because the appendix decompresses after rupture.
Secondary signs become very important. These include loss of the bright submucosal lining, increased echogenicity of surrounding fat, and abscess formation after perforation
Appendicitis Reporting Sample
Finding:
A noncompressible, blind-ending tubular structure is seen in the right iliac fossa arising from the cecal base, measuring 8 mm in diameter with wall thickening and echogenic surrounding fat. A small echogenic focus with posterior shadowing is noted in its lumen suggestive of an appendicolith. Minimal adjacent free fluid is present.
Impression:
Sonographic features are consistent with acute appendicitis with periappendiceal inflammation. No evidence of abscess or perforation at present.