When you scan bowel, most of the time all you see is gas and some tubular fluid filled structures. It is very confusing for beginners. Many people do not know where to start.
In this article, you will learn the most common bowel diseases and how to diagnose them with systematic and practical framework that works very well in real clinical practice.
List of Common Bowel Pathology
- Acute & Emergency
- Appendicitis
- Intussusception
- Bowel Obstruction
- Ileus
- Ischemic Colitis
- Inflammatory
- Diverticulitis
- Infectious colitis
- Enteritis
- Epiploic Appendagitis
- Crohn’s Disease
- Neoplastic
- Colon Cancer
Remember, Ultrasound cannot diagnose every bowel condition.
This list includes about 85 to 90 percent of clinically important bowel diseases that can realistically be detected on ultrasound. Many other conditions are diagnosed using CT, MRI, endoscopy, or histopathology. Ultrasound alone cannot reliably detect all bowel diseases.
Checklist to Diagnose Bowel Pathology in Ultrasound
This checklist provide practical framework that helps to diagnose pathology if you suspect any abnormalities on ultrasound.
- Clinical Clue
- Wall thickness (Symmetrical/Asymmetrical)
- Wall stratification (Intact or Lost)
- Bowel Diameter
- Bowel Peristalsis
- Vascularity
- Compressibility
- Luminal content
- Associated finding
- Fat stranding
- Fluid around lesion or peritoneal cavity
- Lymph node status
We will now discuss each of these points in detail so you will know which important ultrasound features to look for to reach a final diagnosis.
Clinical Clues
Before you start scanning the bowel, you must first look for clinical clues that suggest the probable pathology.
- Patient history
- Investigation finding
- Location of pain
First, ask about the patient’s history and review investigation findings. This will guide you toward the correct differential diagnosis. You’ll know what to look for and where to look.
Next, ask the patient where it hurts the most.
If the patient can clearly point to the most painful area, there is a high chance that the pathology is located there. Carefully examine that area first. After that, scan the rest of the abdomen.
The location of pain can also give you clues about the possible disease affecting the patient. Certain bowel diseases commonly occur in specific areas of the abdomen.
For example, pain in right lower quadrant suggests acute appendicitis. Ileocolic intussusception, which is common in children, usually seen in the right upper quadrant of the abdomen, near the right kidney and the liver. So when you suspect intussusception in a child, you should carefully scan that area.
Bowel Wall Thickness
While scanning, eyeball the wall thickness. Compare it with the adjacent bowel loop. If you suspect it is increased, confirm by measuring it.
- Measure the wall thickness from the outer hyperechoic serosal surface to the inner echogenic mucosal luminal interface.
- Do not include the contents inside the lumen.
- Do not measure from serosa to opposite serosa.
- Measure only a single wall thickness.
- Apply minimal probe pressure while measuring.
Interpretation: wall thickness should be less than 3mm.
If wall thickening is present, determine whether it is symmetrical or asymmetrical.
Symmetrical thickening means the bowel wall is evenly thick all around the lumen. It suggests infection, inflammatory bowel disease, or ischemia.
Asymmetrical thickening means one side of the bowel wall is thicker than the other. The bowel lumen may also appear narrowed. This pattern is highly suspicious for malignancy or a localized tumor.
Bowel Wall Stratification “Gut Signature”
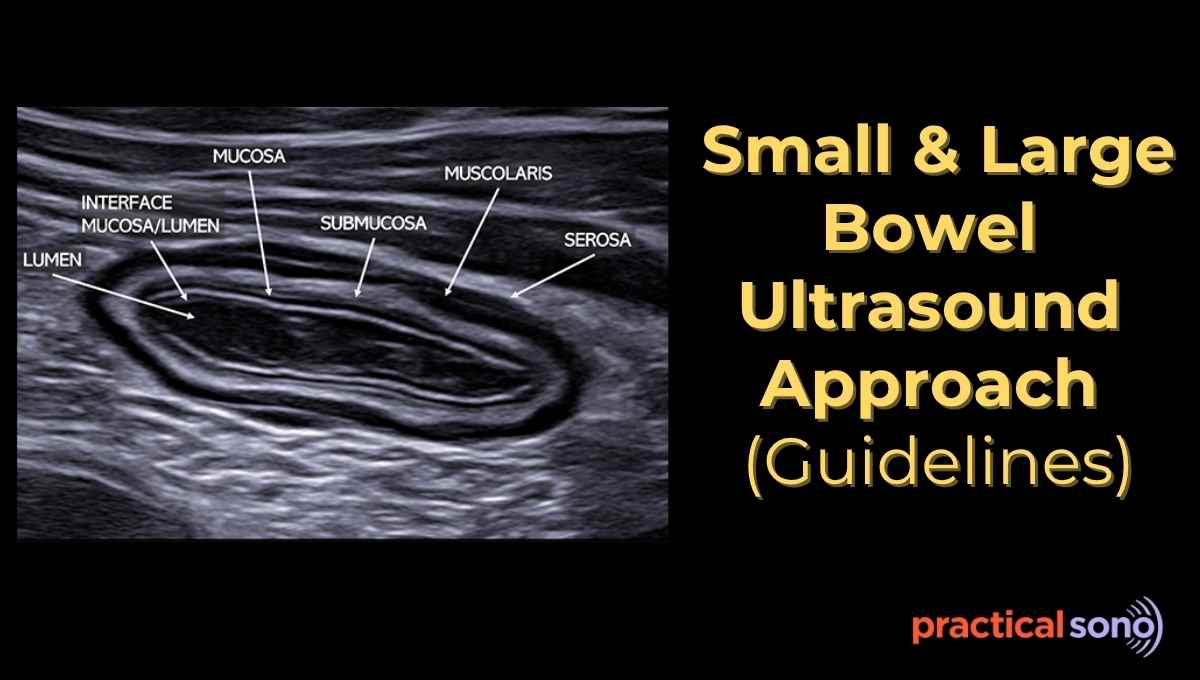
A normal bowel shows five alternating bright (echogenic) and dark (hypoechoic) layers, called the gut signature.
- Echogenic Interface (lumen–mucosa interface)
This is the bright line facing the lumen. It represents the interface between the bowel contents and the mucosa. - Hypoechoic Mucosa
This is a thin, dark layer just beneath the luminal interface. It can thicken early in inflammatory conditions. - Echogenic Submucosa
This is a bright, relatively thick layer. It becomes more prominent when there is edema or hemorrhage. - Hypoechoic Muscularis Propria
This is a dark layer responsible for bowel peristalsis. It can thicken in chronic inflammation or obstructive conditions. - Echogenic Serosa
This is the thin outer bright line. It represents the serosal surface of the bowel.
While assessing the bowel segment, observe the wall stratification. Determine if all five layers of the bowel wall are visible or if the stratification has been lost
Interpretation:
- Thick Wall + Intact Wall Stratification
- Infectious colitis
- Enteritis
- Early inflammatory bowel disease
- Mild ischemia
- Edema
Note: Preserved wall layers means pathology is benign/ inflammatory.
- Thick Wall + Loss of Wall Stratification (Individual layers cannot be distinguished)
- Advanced inflammation
- Severe ischemia
- Malignancy
Bowel Diameter
Next, check whether the bowel is dilated or collapsed.
For the small bowel, the diameter varies depending on meals but is usually less than 2.5 to 3 cm. A diameter greater than 3 cm may suggest an obstruction.
For the large bowel, normal diameters are different.
The colon is usually normal up to 6 cm, and the cecum may measure up to 9 cm. Any dilatation beyond these values suggests obstruction or ileus.
Bowel Peristalsis
Observe the dynamic movement of the bowel loops in real time.
Check for the presence, absence, or exaggeration of bowel motion.
Normal peristalsis appears as smooth, wave-like contractions that push the contents forward.
Hyperperistalsis, or increased motion, can be seen in obstruction or infection.
Hypoperistalsis, or absent motion, may indicate ileus or ischemia.
Any abnormality in peristalsis, whether increased, decreased, or absent, is important. A “to-and-fro” motion is a classic sign of small bowel obstruction.
Vascularity
Normal bowel shows only mild submucosal blood flow. Minimal or no vascular signal is usually detected.
Increased vascularity, or hyperemia, suggests inflammation, such as in Crohn’s disease. Absent vascularity may indicate ischemia or necrosis.
In inflammatory bowel disease, semiquantitative grading systems like the Limberg score can help assess the severity of bowel wall vascularity.
Compressibility
Assess the bowel wall by applying gentle pressure with the probe.
Normal bowel is easily compressible and deforms without resistance.
Non-compressible loops suggest inflammation, fibrosis, mass, or obstruction.
Stiff or decreased compressibility indicates possible tumor infiltration or chronic inflammatory changes.
Luminal Content
Observe the contents inside the bowel.
Fluid appears anechoic (dark), while gas appears as bright echogenic foci with reverberation artifacts. Debris or abnormal content may suggest infection or obstruction.
Dilated loops filled with fluid, gas, or debris can indicate obstruction.
The “small bowel feces sign” refers to particulate matter seen within a dilated small bowel loop, which is a key sign of obstruction.
Associated Findings (Secondary Sign)
Fat Stranding
On ultrasound, fat stranding or “creeping fat” appears as bright, non-compressible tissue surrounding the bowel.
This is a hallmark of active, full-thickness inflammation. The fat reacts to inflammatory signals coming through the bowel wall.
Fluid Around Lesion
Small pockets of dark, anechoic fluid seen next to a thickened bowel segment.
This suggests localized leakage or severe inflammation. It can precede a contained perforation or early abscess formation.
Ascites
Fluid that collects generally in the abdomen, often in the pelvis or around the liver.
While it can result from liver or heart disease, in bowel pathology it usually indicates severe systemic inflammation, protein loss, or generalized peritonitis.
Air Within the Wall
Appears as bright echogenic spots or streaks within the bowel wall layers, sometimes with “dirty” shadowing.
This is a medical emergency. It indicates bowel wall ischemia or severe infection that allows gas to enter the wall.
Lymph Nodes
Enlarged, oval or round, dark structures in the mesentery near the affected bowel.
- Inflammatory: Common in conditions like Crohn’s disease.
- Malignant: Very round, large lymph nodes over 10 mm that lose their fatty center may suggest lymphoma or adenocarcinoma.
Apply this framework while performing a bowel scan. You will definitely find it easier to approach bowel pathology now. Next, read the article, ‘Common Bowel Pathologies Seen on Ultrasound” , which is explained using this framework.